Muscle Twitches — Causes and How to Make Them Stop
Most people ignore the twitches, jerks, and pulses that show up in muscle until they don't go away. From stress to sleep to deeper signals, here's how to decode what your body's trying to tell you.
STORY AT-A-GLANCE
Muscle twitches are extremely common involuntary movements caused by temporary nerve misfiring and usually fall into two categories: fasciculations (small surface-level flickers) and myoclonus (sudden, brief jerks)
Most twitching is benign and linked to everyday factors such as stress, anxiety, poor sleep, stimulant use, dehydration, electrolyte imbalances, or muscle fatigue after exercise
Persistent twitching without weakness is rarely linked to serious neurological disease, while twitching paired with muscle loss, weakness, speech changes, or coordination problems warrants medical evaluation
Not all twitch-like movements are the same — conditions such as hypnic jerks and spasticity arise from different parts of the nervous system and have distinct causes and implications
Many cases improve without medication by supporting nervous system balance through better sleep, reduced stimulants, hydration, mineral-rich nutrition, and relaxation-based strategies
You’re mid-sentence in a meeting when your eyelid starts pulsing. You’re lying in bed when your calf begins twitching. A thumb jumps on its own while you’re scrolling your phone. These involuntary muscle movements can last a few seconds or loop for hours — and once you notice them, they’re hard to ignore.
Approximately 70% of people1 today experience muscle twitches at some point. In most cases, the cause is a tired, stressed, or overstimulated nervous system, and can be resolved with basic self-care. However, a smaller portion of twitches can point to something deeper, depending on what else the body is doing at the same time.
The 2 Types of Muscle Twitches (and What Triggers Them)
Most muscle twitches fall into one of two neurological categories: fasciculations (small surface-level flickers) and myoclonus (sudden, brief jerks). Both involve involuntary movement, but they differ in intensity, origin, and clinical meaning. Fasciculations are more common and usually harmless. Myoclonus, although sometimes benign, can also suggest underlying neurological problems, depending on the clinical context.2
Fasciculations are small, surface-level muscle twitches — These are caused by the spontaneous firing of individual motor units — a motor unit being a single nerve cell and the small bundle of muscle fibers it controls. You’ll usually feel them as a fluttering or ripple just beneath the skin, most often in the eyelids, calves, feet, or arms, and they tend to be most noticeable when you’re sitting or lying still.
Unlike spasms or cramps, fasciculations are not forceful enough to bend joints or affect mobility. They’re often painless and brief, though in some people, they can persist for months.
Common triggers include stress, fatigue, dehydration, and caffeine — These all increase neuromuscular excitability, which essentially means the nerve’s trigger becomes too sensitive and is firing with less provocation than it normally would. Having low magnesium or calcium levels can have the same effect by disrupting the electrical balance that nerves rely on.
You may notice these twitches increasing during periods of anxiety, after strenuous workouts, or following a series of poor nights’ sleep.
Fasciculations are rarely a sign of serious illness — Many people who look for answers about persistent twitching online quickly land on amyotrophic lateral sclerosis (ALS) self-diagnosis, and the worry is understandable. Fortunately, fasciculations on their own — without weakness, muscle wasting, or functional decline — are almost never related to motor neuron disease.
Long-term studies of people diagnosed with benign fasciculation syndrome (BFS) consistently show no progression to ALS or other degenerative conditions. BFS affects approximately 1 in 100 healthy adults, and although the twitches can be persistent and bothersome, again, they are not dangerous.3
Similarly, cramp-fasciculation syndrome (CFS) is a rare condition in which twitching is combined with painful cramps, often in the legs but sometimes in other areas. Symptoms can cause discomfort and fatigue, but do not lead to long-term muscle damage.
On the other hand, myoclonus describes a more dramatic, sudden, shock-like jerk. It can affect a single muscle or an entire region of the body. Depending on the cause, it can be completely normal or a sign of a deeper condition.4 5
Myoclonus is a quick, involuntary jerk or spasm — These movements may be random or repetitive, and they can be triggered by motion, sound, light, or come out of nowhere.
There are two main types: physiologic and pathologic — Physiologic myoclonus occurs in healthy people (e.g., sleep starts, hiccups, or benign twitches in infants). Meanwhile, pathologic myoclonus is associated with conditions like epilepsy, brain injury, metabolic disorders, or neurodegeneration.
Specific subtypes offer diagnostic clues — For example, sleep myoclonus occurs during sleep-wake transitions and is almost always harmless, while action myoclonus is triggered by voluntary movement, such as reaching for a cup. Epileptic myoclonus, on the other hand, is tied to seizure disorders. Stimulus-sensitive forms fire in response to sudden sound or light.
Doctors also classify myoclonus by where it originates in the nervous system — from the brain’s cortex all the way down to peripheral nerves — because the origin shapes both the diagnosis and the treatment approach.
Diagnosis and treatment depend on severity and cause — If myoclonus is frequent or disruptive, a neurologist may order tests such as electromyography (EMG), electroencephalography (EEG), magnetic resonance imaging (MRI), bloodwork, or genetic screening to pinpoint the origin.
Mild physiologic cases like hiccups or occasional sleep jerks typically don’t need treatment at all. However, pathologic myoclonus tied to seizure disorders or neurodegeneration may require more complex treatment.
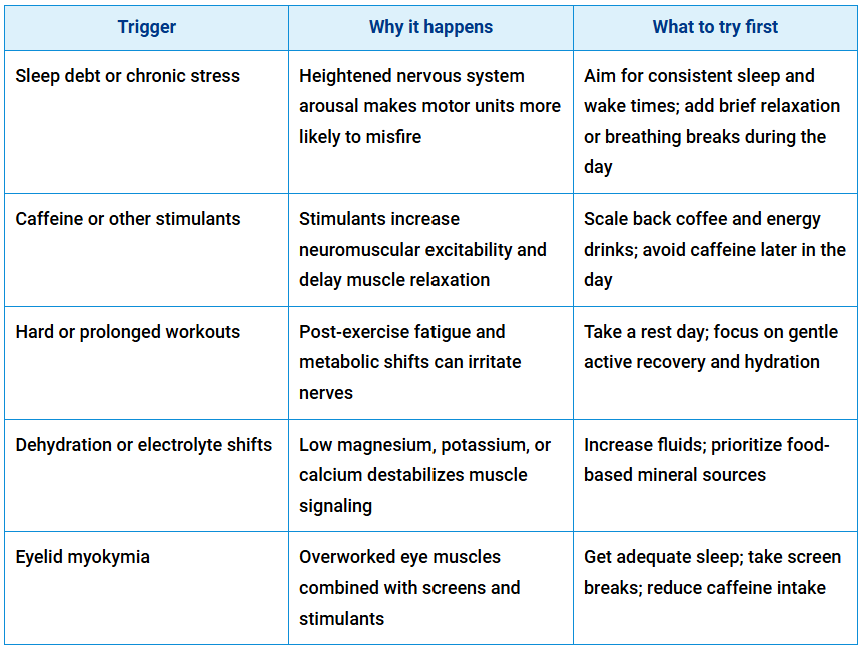
Most muscle twitching is harmless once serious causes are ruled out. Now that you know the clinical names for these movements, the more practical question is: What’s actually triggering them? In most people, the answer is something familiar. This table breaks down the most common everyday triggers:
Other Causes of Muscle Twitches
In addition to the usual causes, other factors can trigger nerve misfires and cause small muscle fibers to twitch. While many of these may seem harmless initially, awareness can help you stay informed.6
Anxiety or stress — There’s a clear biological reason for this phenomenon. When you’re under stress, your body releases adrenaline and cortisol, hormones designed to prepare you for action. One of their effects is to lower the firing threshold of motor neurons, meaning the nerves that would normally remain silent begin to fire spontaneously.
The result is eyelid flickers, facial twitches, or random pulses that seem to come out of nowhere.7 Paying close attention to the twitching can feed the cycle — the more you fixate, the more your nervous system stays on alert, and the more it twitches.
Diuretics and steroid medications — These drugs shift electrolytes or make nerves more excitable, and when nerve fibers become easier to fire, the muscle fibers they connect to may twitch in response.
Nutrient and electrolyte imbalances — Magnesium, calcium, potassium, vitamin B12, and vitamin D all play roles in maintaining the electrical stability of nerve membranes. When any of these nutrients' levels drop too low, nerves become more excitable and may fire spontaneously.
There's also a lesser-known concern worth mentioning — vitamin B6. While B6 supports nerve health at normal levels, over-supplementation — which is surprisingly easy when stacking multiple supplements that each contain it — can cause peripheral neuropathy and contribute to twitching. If you're taking several supplements, check the labels for overlapping B6 content.8
Rare neurological conditions — These are possible but usually come with other symptoms. While disorders affecting the lower motor neurons, such as ALS, post-polio syndrome, spinal muscular atrophy (SMA), or progressive muscular atrophy, can cause twitches, they almost never appear alone.
Twitching in ALS, for example, typically occurs alongside weakness, muscle wasting, cramping, balance problems, a weak grip, slurred speech, or tongue twitching. These conditions are uncommon, and twitches without additional symptoms are rarely related to them.
Beyond the Typical Twitches
Most twitching falls into the categories above — nerve fatigue, stress, minerals, or medications. But not all involuntary muscle movements are twitches in the clinical sense.
Hypnic jerks feel like falling as you fall asleep — Also called sleep starts, these are brief, involuntary jolts that happen during the transition into sleep. They may be accompanied by vivid dreams or a sensation of tripping.
Most people don’t even remember hypnic jerks, but in some cases, they can trigger sleep anxiety or repeated awakenings. If they happen frequently, reducing stimulants, improving sleep hygiene, and managing stress often helps. Learn more by reading “Do You Have Hypnic Jerks?”
Spasticity involves stiffness, not twitches — Unlike fasciculations, spasticity results from impaired nerve signaling between the brain and spinal cord. This causes continuous muscle tightness or sudden spasms. It’s common in neurological conditions that affect upper motor neurons, like multiple sclerosis (MS), cerebral palsy, and spinal cord injuries.9
Twitches and spasticity come from different places in the nervous system — Think of your motor system as a two-part relay. Upper motor neurons run from the brain down through the spinal cord — they’re the command center that decides how much muscle tone to allow. Lower motor neurons pick up those signals and carry them toward the final stretch to your muscles.
Fasciculations arise when lower motor neurons misfire at that final stretch. On the other hand, spasticity occurs when upper motor neurons lose their ability to regulate tone, causing muscles to remain tight or to spasm involuntarily.
Some twitch-like sensations don’t fall neatly into known categories. Middle ear myoclonus can cause clicking sounds when facial muscles spasm. Palatal myoclonus involves rhythmic soft palate contractions. These rare cases often involve focal nerve dysfunction and may require specialty treatment.
When to See a Health Care Provider
This section explains how to distinguish fasciculations from cramps, spasms, and tremors, and when a pattern or symptom might warrant a visit to your physician.10
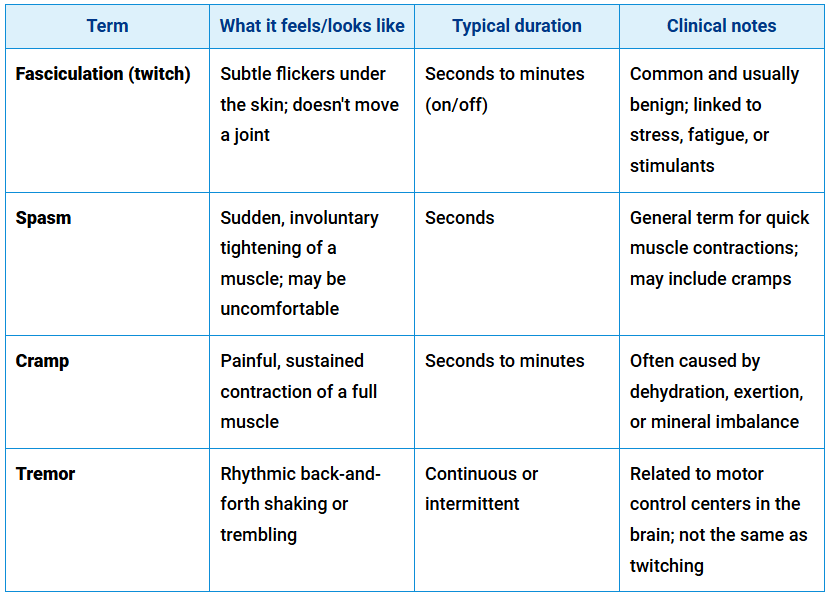
Many people describe any strange muscle sensation as a “twitch,” but that’s often not accurate. True fasciculations differ from cramps, spasms, and tremors — and knowing the difference helps guide what to monitor or mention to your doctor. Here’s a quick breakdown.11
When to seek professional help — If you notice the following, it’s time to check in with a health care provider:12
Twitching lasts more than two to three weeks without relief or a clear cause
The twitching is focal and repetitive in one specific area
You notice accompanying symptoms, such as muscle weakness, atrophy (shrinking), cramping, slurred speech, or poor coordination
You suspect it’s medication-related or linked to recent illness
There’s a family history of neurological conditions
Possible interventions — If needed, your health care provider may refer you for EMG, nerve conduction studies, or MRI to rule out underlying neurological or metabolic causes.
How to Calm Muscle Twitches
If you’ve ruled out red flags or your doctor has confirmed benign twitching, the focus shifts to calming a nervous system that’s running a little too hot. Most muscle twitches resolve with basic care that supports a well-regulated nervous system:13
Make sleep and stress management a priority — Try to get eight hours of good sleep each night. Being tired or overwhelmed is one of the most common reasons muscles start firing off on their own because both lack of sleep and chronic stress make the nervous system jumpier.
Cut back on stimulants and keep yourself hydrated — Too much caffeine or nicotine can overstimulate your motor nerves and make twitching more noticeable. It often helps to ease up, especially later in the day. Drinking water regularly also helps maintain the proper function of the muscles and nerves.
Give your body time to recover after hard workouts — Tough or long exercise sessions can leave motor neurons tired, which is why twitches sometimes show up hours or even days later. Rest days, lighter movement, or gentle active recovery can go a long way in helping your muscles reset.
Know when it’s time to check in with a doctor — If twitching sticks around for more than a few weeks, starts spreading, or comes with weakness or muscle loss, it’s worth getting evaluated. It’s usually nothing serious, but persistent or changing symptoms deserve a closer look.
Natural Ways to Manage Muscle Twitches
Most muscle twitches don’t need medication. Whether caused by stress, fatigue, or overstimulation of the nervous system, from simple sleep hygiene to magnesium-rich foods and relaxation tools, these strategies support the body’s repair systems without relying on drugs.
Stock up on magnesium — Also known as the “recovery mineral,”14 magnesium acts as a gatekeeper for nerve activity. It helps regulate the flow of calcium into nerve cells, and calcium is what triggers a nerve to fire. When levels drop, that gate swings open too easily, leading to twitching and even painful cramping.
Magnesium-rich foods include dark leafy greens, bananas, beans, and dark chocolate. If you suspect a deficiency, your doctor can check your levels and suggest supplementation — magnesium glycinate is a gentle, well-tolerated form especially before bed.
If you have hypnic jerks, try these relaxation techniques — Frequent sleep starts or “hypnic jerks” can be disruptive and anxiety-provoking. While they’re harmless for most people, stress about them can exacerbate them. Try these activities to help you and your muscles calm down:
Guided imagery or progressive muscle relaxation
Breathing exercises and self-hypnosis
Tai chi or yoga
Meditation or biofeedback-assisted relaxation
Calming music or lavender essential oil
Autogenic training (focusing on sensations in the body)
Use nutrition to calm inflammation and support recovery — Foods rich in antioxidants and muscle-supportive nutrients, such as tart cherry juice, blueberries, protein, curcumin-containing spices, and pomegranate juice, can help reduce twitching and muscle tension over time.15
Frequently Asked Questions (FAQs) About Muscle Twitches
Q: Why do my muscles twitch even when I’m resting?
A: Muscles can twitch at rest when the nerves controlling them fire on their own. This often happens after exercise, during stress, or when you’re overtired. Most resting twitches are harmless and fade without treatment.
Q: When does muscle twitching become something to worry about?
A: Twitching becomes concerning when it appears with muscle weakness, shrinking muscles, trouble speaking or swallowing, or symptoms that keep spreading. When those show up together, it’s best to get medical evaluation.
Q: Can stress or anxiety really cause muscle twitches?
A: Yes. Stress and anxiety increase adrenaline and nerve excitability, which can trigger eyelid flickers, facial twitches, or random pulses in different muscles. These usually calm down once stress levels ease.
Q: Can low magnesium, calcium, or vitamin B12 cause muscle twitching?
A: Low magnesium, calcium, or vitamin B12 can make nerves fire unevenly, which may cause twitching. These deficiencies are typically easy to identify and correct with diet changes, supplements, or medical evaluation.
Q: Are muscle twitches a sign of amyotrophic lateral sclerosis (ALS)?
A: Twitching by itself is rarely a sign of it. In ALS, twitches usually come with muscle weakness, difficulty activating muscles, or visible muscle wasting. Most isolated twitches are benign.
Disclaimer: The entire contents of this website are based upon the opinions of Dr. Mercola, unless otherwise noted. Individual articles are based upon the opinions of the respective author, who retains copyright as marked.
The information on this website is not intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice. It is intended as a sharing of knowledge and information from the research and experience of Dr. Mercola and his community. Dr. Mercola encourages you to make your own health care decisions based upon your research and in partnership with a qualified health care professional. The subscription fee being requested is for access to the articles and information posted on this site, and is not being paid for any individual medical advice.
If you are pregnant, nursing, taking medication, or have a medical condition, consult your health care professional before using products based on this content.